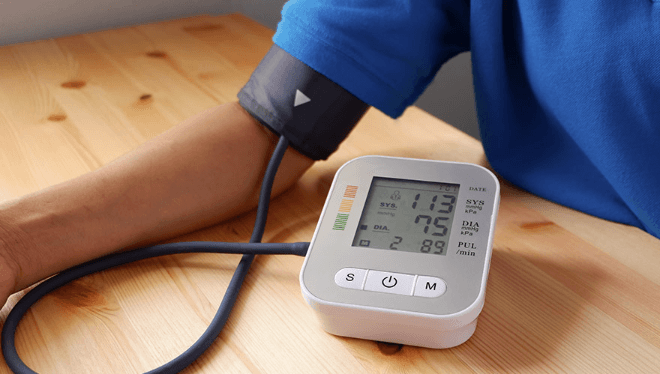
Smart medical devices are digital tools that aid diagnosis, monitoring, and treatment through continuous data streams from sensors and secure connectivity. They rely on data validation, time-stamped communications, and sensor fusion to improve accuracy, while enabling remote care and real-time decisions. Their usefulness comes with privacy, cybersecurity, and autonomy concerns. Effective use requires governance, interoperability, and ongoing maintenance. As clinicians and patients weigh benefits and risks, the practical questions of ownership, consent, and data sharing become pivotal. The next layer of detail awaits.
What Are Smart Medical Devices and Why They Matter
Smart medical devices are digital or connected tools that assist in diagnosing, monitoring, treating, or preventing health conditions. They enable remote care, data-driven decisions, and agile responses within systems that value autonomy.
The field faces privacy concerns and regulatory challenges, requiring transparent risk assessment and interoperable standards to preserve safety while expanding patient choice and practical, evidence-based innovation.
How They Work: Data, Sensors, and Connectivity
Data, sensors, and connectivity form the backbone of smart medical devices, enabling continuous sensing, real-time analysis, and secure data transfer across care settings. These systems rely on robust data protocols to validate, timestamp, and encrypt streams while preserving interoperability.
Sensor fusion integrates disparate inputs to improve accuracy, enabling reliable alerts and decisions even amid noisy measurements.
Benefits and Risks for Patients and Clinicians
The benefits and risks of smart medical devices for patients and clinicians emerge from how continuous sensing, real-time analysis, and secure data exchange influence care workflows and outcomes.
These technologies can improve monitoring, early intervention, and efficiency, but introduce privacy concerns and potential dependence on automated judgments.
Respecting user autonomy remains essential to maintain trust, choice, and informed decision-making in care.
Choosing, Using, and Evaluating Smart Medical Devices
Decision criteria weigh reliability, interoperability, and cybersecurity.
Practitioners assess ongoing maintenance, clinician training, and patient engagement.
Privacy concerns and data ownership shape consent, access, and sharing.
Transparent vendor transparency, independent testing, and post-market surveillance support informed, freedom-centered device selection and utilization.
Frequently Asked Questions
How Secure Is Data From Smart Medical Devices Against Breaches?
Data from smart medical devices is safeguarded through data encryption and regular firmware updates; however, experts note persistent breach risks from zero-days, supply-chain flaws, and user error, demanding layered security, continuous monitoring, and transparent disclosure for informed freedom.
Can Smart Devices Replace Routine Clinician Visits Entirely?
Remote monitoring cannot fully replace visits; humans still require complex assessments. Can remote monitoring replace visits, yet ethics of autonomous care demand safeguards, oversight, and transparency to preserve freedom while ensuring safety and evidence-based care.
See also: kuttymovies7
What Costs Are Involved Beyond the Purchase Price?
Costs extend beyond purchase: data ownership implications, ongoing maintenance, software updates, cybersecurity, telemetry fees, interoperability considerations, support contracts, and potential integration with existing systems—all affecting total value and freedom to choose among interoperable, secure solutions.
How Do Devices Handle Power Outages or Battery Failures?
Power resilience is built into systems with uninterruptible power, backup batteries, and failsafe modes; devices switch seamlessly, alert staff, and log outages for maintenance. Battery maintenance schedules and diagnostics ensure continued operation during outages and power quality issues.
Are There Age or Disability Limitations for Device Use?
The answer: There are age limitations and disability considerations vary by device, with many models offering accessibility features; manufacturers provide guidelines and clinicians tailor use, ensuring safety, efficacy, and user autonomy through customized settings and progressive adoption.
Conclusion
Smart medical devices represent a data-driven frontier for vigilant, proactive care, but their promise depends on rigorous governance and interoperability. When properly implemented, they enable continuous insight, timely interventions, and personalized support. Yet concerns about privacy, cybersecurity, and autonomy persist; these require robust consent, secure architectures, and transparent usage policies. Overcoming the objection that more data automatically equates to better care, the text asserts that quality depends on context, governance, and clinician–patient collaboration, not raw data volume alone.